What is it?
The soft tissues in your hand and fingers are arranged in special layers. The layer just under your skin but above your tendons is called fascia. The fascia is in the hand to help bind the skin in place during grip. Without it the skin of the fingers would slide around during grip. It is normally a thin layer. In Dupuytren’s disease the fascia changes its behaviour. It gets thicker, forming lumps and cords in the palm and fingers. Any cords that form can shrink. This causes the fingers to be pulled over. If the fingers are left bent they can become permanently stiffened.
What causes it?
There is a strong family linkage to this disease but in most cases we do not know why people get this problem. Sometimes the cause can be traced to diabetes, liver disease smoking or alcohol intake. At present we do not think there is a link between Dupuytren’s disease and work. Dupuytren’s disease commonly gets worse over time. In some people it gets worse very quickly, in others it changes very little over the years.
How do you know that I have it?
An assessment in clinic is usually enough to tell you have Dupuytren’s disease. Special tests are not usually needed. Sometimes it is even possible to predict how severe your problem is from the history and examination alone.
Can it be successfully treated without surgery?
Injections of steroid in to the lumps can give pain relief in minor cases when there is pain. This is uncommon. In addition, please refer to the Patient Information topic “Dupuytren’s Disease (Non-Surgical Treatment)”.
When will I need surgery?
If your Dupuytren’s is causing your fingers to bend up a lot (see pictures below) or if it is causing you functional disability you will be offered an operation. There is a reliable operation, which corrects Dupuytren’s disease in over 90% of cases. This operation is called a fasciectomy. What you need to know is that Dupuytren’s disease can come back after surgery. This is called recurrence. Recurrence will occur in about half of patients, but is usually very slow. About one in ten patients will not have successful surgery or will have a recurrence soon after their surgery. I cannot predict who will get recurrence before I operate.
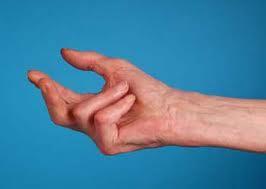 |
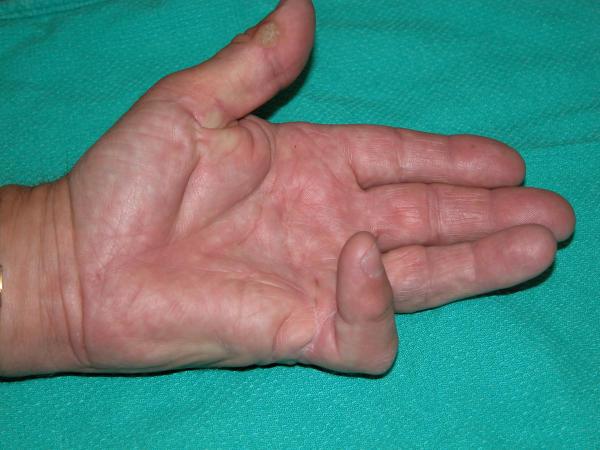 |
What happens in a fasciectomy?
Patients usually have the operation as a day case. This means they come to hospital, have the operation and go home all in the same day. They may not have to go to sleep. Instead, the arm is numbed with an injection into the neck or around the shoulder. An inflatable bandage (like a blood pressure cuff) is put round the arm, this is called a tourniquet and it stops bleeding during the operation. A zigzag cut is made in the hand over the disease and the Dupuytren’s tissue is removed. The nerves and the blood vessels of the fingers are very close to the diseased tissue and may be damaged during surgery. After removing all the tissue the joints of the finger may need to be released. Skin grafts are needed in about 1 in 20 cases. The graft is quite small and is usually taken from your forearm. The wound is then stitched up. The hand is bandaged with a plaster of Paris splint.
After the operation a sling is provided. This keeps the hand up and cuts down on swelling. It is best to keep the hand in the sling when upright, or, raised on pillows when lying for the first two days. The post-operative dressings are replaced with a removable splint after two or three days and physiotherapy is commenced. Using the hand as normally as possible speeds recovery. The hand must be kept clean and dry. The stitches are taken out at 10-14 days after the operation. The ward staff will arrange this. Driving is not normally allowed until the stitches have been removed. If there have been no complications there will be no limits on what you are allowed to do after the stitches are removed. You will be asked to wear a splint on your finger at night for six months after surgery.
Time off work is usually 2-7 days for people in light work and 2-6 weeks for people in heavy, dirty work. People working with food are not allowed back to work until the wound is completely healed.
What are the complications of fasciectomy?
Infection – the most common, usually easily treatable with antibiotics.
Nerve injury – bruising injury is as common as 10% of cases, but gets better without treatment. Permanent injury is rare but serious. Usually treated by surgery to the nerve.
Vessel injury – very uncommon but serious. If the blood supply to the finger does not recover the finger may need to be removed at a later date.
Stiffness – if you had joint releases at surgery then your fingers may be stiff. Most simple cases do well without physiotherapy. You are encouraged to move the fingers as much as possible after surgery.
Dystrophy – extremely rare but serious complication in which the whole hand gets very sore and seizes up. It can be treated but treatment can take a long time and the hand may be stiffened at the end.
Recurrence – not strictly a complication. Commonly the scar is tender for some months afterwards. This is normal and will go away. Massaging with moisturising cream will help.